We’re used to thinking of COVID-19 testing as an activity that is led by government public health agencies, supported by private testing laboratories such as Quest Diagnostics and LabCorp.
But American businesses have a broader role to play. Workplace-based testing for COVID-19 infections is shaping up to be a crucial component of managing the virus and getting the economy restarted again.
In mid-April Scott Gottlieb, former head of the FDA, wrote a op-ed (1) for the Wall Street Journal where he argued that:
Government policy can encourage employer-based testing in two ways. First, without cutting corners, federal and state regulatory agencies should be open to approving employer-based testing laboratories that will add significantly more national testing capacity. Second, the U.S. should consider subsidizing sick leave for workers that test positive, in order to encourage more companies to do testing.
Oddly enough, the CDC is still treating testing as a scarce resource, as it has since the beginning of the pandemic, and actively discouraging employer use of tests. The current CDC guidelines (2) for employers suggest checking workers for virus symptoms or elevated temperatures, but goes on say: “[e]mployers should not require a COVID-19 test result ….to return to work.”
But to be polite, that attitude from the CDC misses the point. President Donald Trump has explicitly made testing the responsibility (3) of state governments, in conjunction with the leading private labs, and they simply don’t have the resources to carry the whole load. It’s time to harness the financial heft of the business sector to pick up some of the testing burden.
Even in the face of CDC discouragement, companies such as Amazon, U.S. Steel (4), Whirlpool (5), Microsoft, Intel and Las-Vegas based Wynn Resorts are either considering or already exploring (6) workplace-based testing. Amazon (7), in particular, is taking steps towards (8) setting up its own laboratory facilities in order to regularly test all staff, including those without symptoms, according to CEO Jeff Bezos in his letter to shareholders. According to its latest earnings report, the company expects to spend “hundreds of millions” of dollars in the second quarter to develop its own COVID-19 testing capabilities.
What are the pluses and minuses of workplace-based testing? Done right, it benefits workers, businesses, and the broader society. Individuals get a safer work environment and sick leave if they test positive. Businesses get to stay open in a sustainable way. And public health is improved, especially if the information gained from the test can be used to inform contact tracing. It becomes a bridge to broader testing. Workplace testing gets us a lot closer to the 500,000(9) to 1,000,000 (10) tests per day that many experts think are necessary.
Done wrong, workplace-based testing can be used as a hammer against workers, violating privacy without gains. The key is to understand what workplace-based testing can do and what it can’t.
It’s important to realize that we’re talking about tests for current COVID-19 infection, not tests for antibodies or immunity. Some people have suggested favoring workers who have coronavirus antibodies, but it’s going to be some time before we know how long immunity (11) lasts. As long as that’s unknown, companies have to test for infections, not antibodies.
A company that wants to do workplace-based testing has two key decisions. First, will the tests be voluntary or mandatory? The safest thing for workers is to test everyone at regular intervals, but that’s more expensive.
Companies also need to choose whether to contract for third-party testing services, to buy tests for use in in-house clinics, or to actually set up their testing laboratories. Most businesses will choose one of the first two options. Currently, each cartridge for Abbott Laboratories’ rapid coronavirus tests costs (12) $40. The Cepheid point-of-care test requires a cartridge (13) that sells for $35. In addition, companies have to figure in the cost of the equipment and trained personnel to administer and run the tests. Medicare is reimbursing as much as $100 per test. (14)
But these numbers will likely come down quickly as more tests come on the market. Big companies can buy in bulk, which can help bring down the costs.
Moreover, the largest companies have the financial strength and incentive to set up their own lab facilities, if they choose. That would add new testing capacity to the United States and take the pressure off both the supply of tests from manufacturers and off the leading private labs. LabCorp and Quest Diagnostics are both in the Fortune 500, but they are dwarfed by companies such as Amazon, Walmart, Target and even Tyson Foods, which has been hit by outbreaks (15) at some of its meat-processing plants.
One reason for large companies to choose the third option– setting up their own lab facilities— is economies of scale. COVID-19 is not going away, and the nasal swabs or saliva (16) analysis will have to be repeated regularly, both because of the possibility of false negatives and because workers can obviously pick up the coronavirus at home or in the community. At the volumes needed, it wouldn’t be surprising to see the marginal cost per test drop to $10-$20 per test. (that’s the added cost of running an additional test, not including capital costs).
Setting up a testing lab is not a one-day process, by any means. Companies that go this route have to hire a lab director and other professionals, buy lab equipment, and get CLIA (Clinical Laboratory Improvement Amendments) certification from the federal and appropriate state governments. The new labs also have to develop their own testing protocols for COVID-19, and get them approved, though that will be easier as more companies go this route.
None of these steps are true blockers for a motivated company that want to do this. But they do require the company to invest some money, and involves going through a regulatory approval process for each state where testing is done. State governments can help by encouraging companies to invest in testing laboratories that add more capacity.
However, as an economic and social decision, workplace testing is a positive for both employees and employers. Everyone wants to earn a living, and no one wants to die. So workplaces that pay more attention to safety will be more attractive to workers, especially if a positive test comes with paid sick leave and payments for care.
Similarly, as the cost of testing goes down, it looks increasingly appealing from a business perspective as well. A large body of economic literature (17) on the risk-pay tradeoff implies that businesses that don’t test will have to pay significantly higher wages in order to attract workers, even in these hard times. Workers have a good sense of their risk level, and vote with their feet accordingly. By contrast, businesses that implement an effective testing strategy will find themselves able to run their operations more efficiently and profitably, while protecting their workers.
The largest businesses are likely to be the ones that lead the way towards testing. Let’s do an illustrative calculation. Pre-pandemic, there were roughly 1400 firms with employment over 10,000 workers in the United States. Together these firms employ roughly 30 million workers. Not every big company will test, of course, but if 20% of these big-company workers are tested every two weeks, on average, that comes to an average 400,000 tests per day. Assuming a marginal cost of $10-$20 per test, that comes to $4-$8 million per day. That’s on top of the sizable capital cost of setting up the testing laboratories. (Amazon’s large outlays partly reflect the costs of being the pioneer in this area).
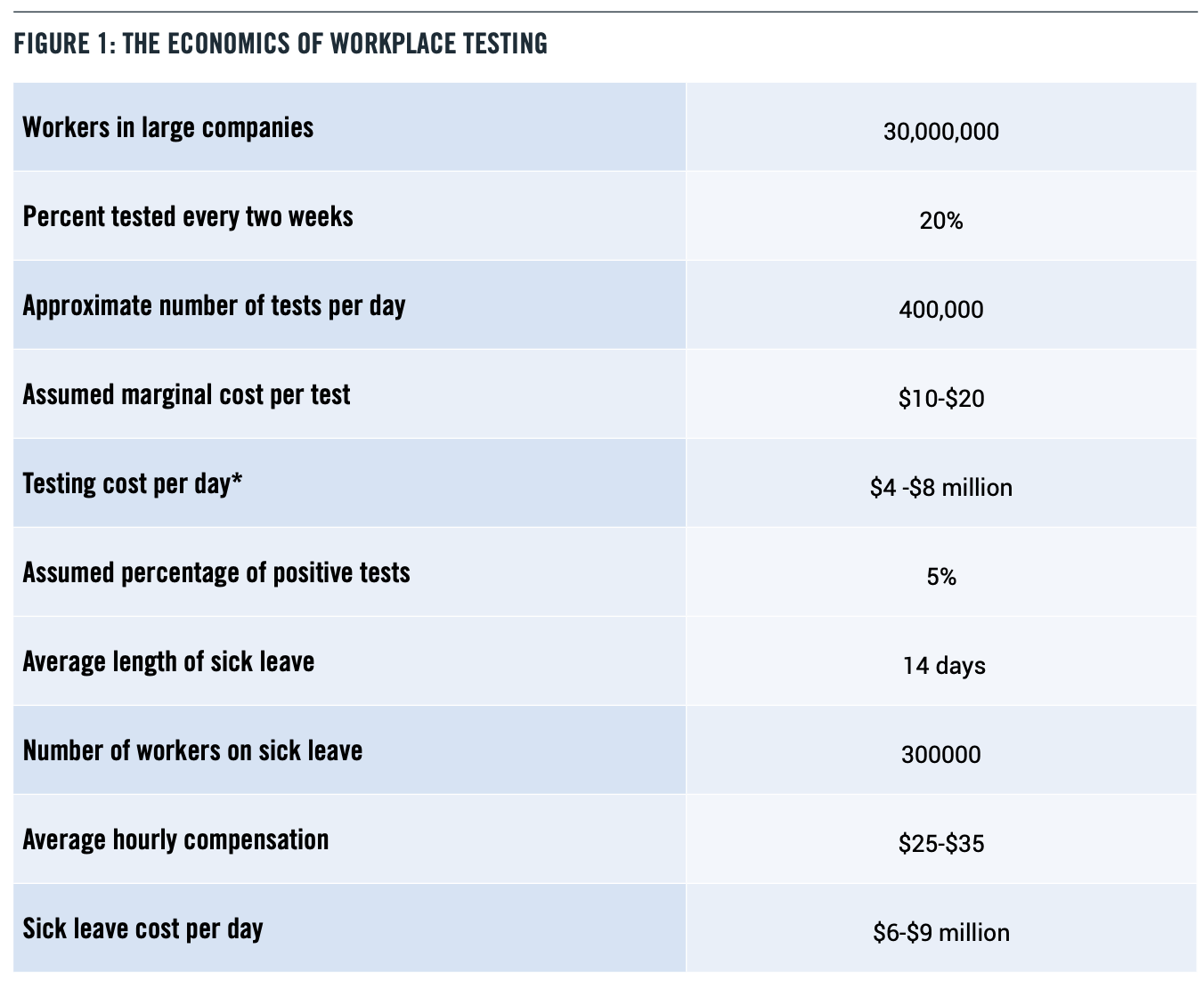
In addition, workers that test positive should be eligible for paid sick leave, probably averaging two weeks. That’s likely to raise payroll costs more than the testing itself. If we assume that 5% of the tests come back positive, that’s 300,000 additional workers on sick leave at any time. Assuming average compensation costs of $25-$35 per hour that raises annual compensation costs to large companies by $6-9 million per day. That’s a significant cost, but it can be absorbed or passed onto consumers as an essential part of doing business.
To be a good proposition for workers and businesses, testing doesn’t have to be perfect but it does have to be systematic. Businesses can’t stop and start — they have to pick a strategy and stick to it. And the strategy has to include a commitment to take immediate steps when positives occur, as they inevitably will.
It should be noted that there’s one part of the labor market where the risk-pay tradeoff doesn’t hold, and that’s immigrant workers, especially from Mexico. According to a 2010 economic study (18), Mexican immigrant workers “on average receive zero or very low levels of wage premiums for fatal injury risks.” The key factor appears to be whether the immigrant worker is fluent in English. So industries that employ a larger number of Mexican immigrants who are not fluent in English — notably agriculture and food production — may not be under the same pressure to test. That suggests a need for special scrutiny by state and local governments.
Legally, testing by employers (19) is on firm ground during a pandemic, as part of providing a safe workplace. The EEOC has noted that:
In addition, the EEOC has noted that while employers must keep health records in a confidential file, they may disclose the name of employees that have COVID-19 to public health authorities.
That’s important. The information from the tests has to be available to the public health authorities for contact tracing and potential isolation of infected people.
While much of testing can be decentralized to workplaces, contract tracing and followup is something only the public sector can take the lead on, aided perhaps by the sort of technological capabilities that companies such as Apple and Google are building.
The public health system needs to be ready to act on the information garnered from employer testing with sustained contact tracing, to understand how the worker got infected and to potentially isolate their families and contacts who may be asymptomatic and not realize that that they are infectious. So business testing makes sense as a complement to investment in public health contact tracing as well.
The government can give businesses an incentive to do the right thing by subsidizing sick leave that is the result of a positive test. That would encourage more companies to test their workers.
The government could also help by finding a way to streamline the approval process for corporate testing labs in multiple states, in response to the pandemic. Simply having the CDC come out in favor of workplace testing would make things easier. And while the EEOC statement is reassuring, it may also be helpful for Congress to address potential liability issues connected with employer testing, which is the right thing for workers.
What about the downsides of workplace-based testing? It clearly raises issues of privacy, especially if the names of people who test positive are passed onto public health authorities. It’s essential that workers not be penalized for testing positive. Nor should they be penalized for being in a vulnerable category, like being over 60 or immune-compromised. Indeed, comprehensive testing makes it easier to employ such people.
Another issue is whether small businesses can afford workplace-based testing that allows them to compete with big businesses. Some provision should be made for allowing small businesses to take advantage of the testing supply chains that large companies develop, perhaps by giving them access to low-cost testing.
In the end, testing in the workplace is an affordable proposition. It will raise costs and likely prices, and lower profits, but that’s a small price to pay for a safer workplace. President Trump is eager to reopen the U.S. economy. But he doesn’t seem to understand that will require much more testing that we are doing today. Sustained business testing will take a significant burden off the public health system. If a significant number of large employers start workplace testing, it has the potential for reaching a large number of Americans quickly. It’s the right thing for businesses to do.
PPI_How-Workplace-Testing-Can-Get-Us-Back-to-Work